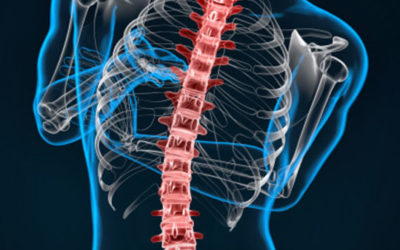
At Essendon Chiropractice Centre, we provide assessment and treatment for patients with spinal injuries or bad spinal conditions including:
- Scoliosis
- Joint Dysfunction
- Spinal Impairment
We work with the clients and their families for building skills and support strategies to reduce impairment and enable more independence. Here are few knowledge articles that may help:
Scoliosis
Scoliosis is a disorder that causes an abnormal curve of the spine, or backbone. The spine has normal curves when looking from the side, but it should look straight when looking from the front.
Temporomandibular Joint
The Temporomandibular Joint (or TMJ) is the joint that connects the skull with the jaw. The TMJ is a complex joint that is connected by muscles inside and outside the jaw
Clinical Pilates
Clinical Pilates is an individually designed strengthening and stretching program that is receiving worldwide recognition for its use in the rehabilitation of musculo skeletal injuries…
Adolescent Spinal Curvature
Adolescence is a critical time for spinal health. The postures and habits of your children from 10 to 15 years of age will determine the health or ill health of their spine for the rest of their lives…